The lack of medicines in Europe is not a simple logistical failure nor a production problem. It is the symptom of systems blind to actual demand behavior. And that disconnection is silently redefining the role of the pharmacist.
By Ehab Soltan
HoyLunes — For years, the shortage of medicines in Europe has been explained through a widely documented set of factors: supply chain disruptions, manufacturing dependence on third countries, seasonal demand spikes, or geopolitical tensions. All these causes are true. None are sufficient to explain the persistence of the problem.
What is emerging in 2026 is a more uncomfortable, structural, and purely operational hypothesis: the shortage is not solely a physical lack of supply, but a systemic desynchronization between how medicine is prescribed, distributed, and consumed in contemporary reality. This misalignment is not conceptual; it is measurable, operational, and potentially correctable.
The European pharmaceutical system is not failing due to a lack of raw resources, but rather due to a profound lack of alignment with actual patient behavior. This explanatory framework has been useful, but is insufficient to explain the persistence, recurrence, and irregular distribution of the phenomenon in highly regulated systems.

The Ghost Patient: When the Traditional Model Ceases to Exist
The traditional forecasting model assumed a linear and relatively stable flow: the doctor prescribes, the pharmacy dispenses, the patient consumes. That world no longer exists.
Today, patient behavior is dynamic, fragmented, and often invisible to data systems:
Changes treatment based on immediate availability in the pharmacy.
Interrupts therapies due to mistrust, misinformation, or unreported side effects.
Consults multiple sources (digital, private, international), altering their purchasing route.
Anticipates purchases and accumulates personal stock in the face of shortage rumors.
Adjusts dosages on their own without medical supervision.
This new “ghost” behavioral pattern is not integrated into forecasting algorithms. The result is systemically inefficient: the system calculates a theoretical demand based on historical data, while actual demand moves in a completely different direction in operational time. This divergence introduces cumulative errors in forecasting, distribution, and replenishment that the current system is not designed to correct.
The 2026 Hypothesis: Fracture Between Registered Demand and Actual Need
The central thesis is sharp: Europe does not suffer shortages because molecules are missing, but because systems are not designed to capture actual demand in operational time.
This generates three simultaneous fractures that paralyze the chain:
Clinical Demand vs. Actual Demand
What the doctor prescribes on paper is nowhere near what the patient ends up consuming.
Registered Demand vs. Anticipated Demand
Logistical systems react late because they operate looking in the rearview mirror of historical data, blind to present behavioral changes.
Logistical Availability vs. Actual Accessibility
The medication may exist physically in a central warehouse… but it is not where or when the patient desperately needs it.

The Critical Point: The Pharmacist as a Sensor No One Is Listening To
In this scenario appears the most undervalued and, paradoxically, the most crucial actor in the system: the pharmacist.
The pharmacy is the only convergence point where medical prescription, patient final decision, effective availability, and the need for substitutions or adjustments meet in real time. However, this granular and precious knowledge is not structurally integrated into the healthcare system.
The pharmacist detects desynchronization patterns before any algorithm:
Identifies medicines that suddenly stop being requested.
Manages recurring substitutions that indicate an imminent supply failure.
Observes patients who do not complete chronic treatments.
But this crucial knowledge remains trapped at the counter. It does not scale. It does not inform. It does not transform the system. It is wasted intelligence. Integrating this intelligence does not require reinventing the system, but recognizing the pharmacist as an active node within the healthcare decision-making architecture.
The Operational Paradox: More Digital Health, Less Real Visibility
Europe has made gigantic progress in digital health, but with a critical bias that perpetuates blindness:
Prescription has been digitalized (e-prescription).
Medical records have been digitalized.
Logistical traceability has been digitalized.
But neither patient behavior nor the critical decisions occurring at the point of dispensing have been effectively digitalized. The system continues to operate under the erroneous premise that clinical data is sufficient to forecast demand. It is not.
The European Medicines Agency itself has pointed out that supply problems cannot be understood solely from production, but from usage and demand patterns.
(More information at: [[https://www.ema.europa.eu/en/human-regulatory/post-authorisation/availability-medicines])
The Structural Error: Attempting to Manage Chaos with Static Tools
The current European pharmaceutical system was designed for a context that has disappeared: predictable demand, passive patient, and linear flows. The problem is not lack of capacity, but the lag between system architecture and environmental behavior.
Today we operate in a radically different environment where information alters patient behavior in real time, mistrust influences adherence, and perception of availability modifies demand. Attempting to manage this dynamic environment with static models generates an inevitable effect: perceived shortage and operational chaos, even when physical supply exists. This misalignment is not theoretical; it already translates into tangible operational pressure brutally impacting the three key actors:
Pharmacists: Are forced to be managers of uncertainty and rationing, assuming indirect clinical decisions (substitutions), and facing patient frustration, losing vital operational time.
Distributors: Operate blindly, managing unforeseen demand peaks with incomplete data, assuming reputational and economic risks without actual control.
Patients: Perceive constant insecurity that further alters their behavior (stockpiling, abandonment), irreversibly damaging therapeutic adherence.
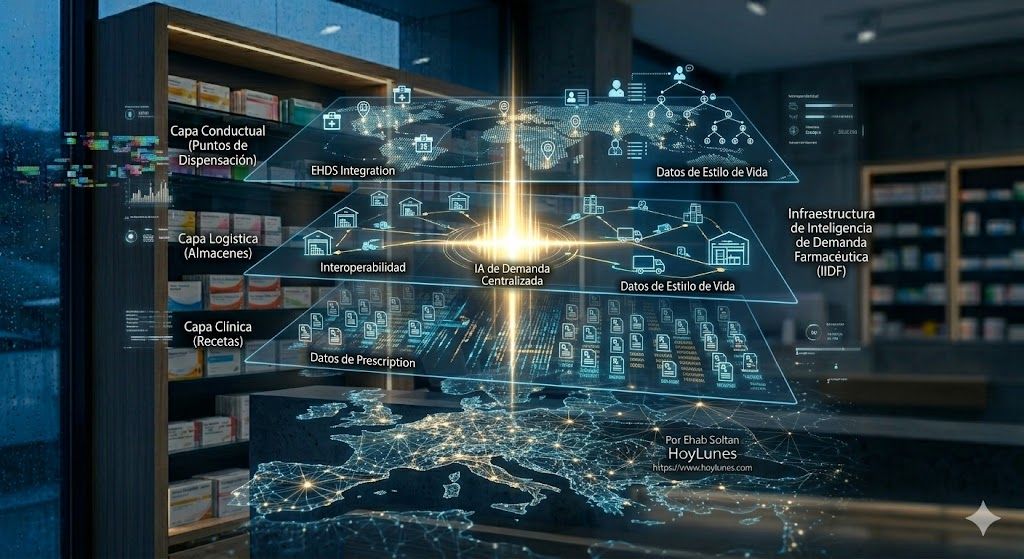
The Invisible Opportunity: Real-Time Pharmaceutical Intelligence Infrastructure
This is where the problem stops being clinical and becomes a strategic opportunity. The solution to shortages in Europe is not simply to produce more. It is to interpret better.
Europe urgently needs a new layer of technological infrastructure: a Pharmaceutical Demand Intelligence Infrastructure. A system capable of:
Anonimized capturing of decisions and frictions at the point of dispensing.
Integrating actual patient behavior into forecasting models.
Detecting demand deviations in real time.
Anticipating supply tensions before they become stockouts.
Dynamically providing feedback to doctors, distributors, and manufacturers.
This layer not only optimizes the system; it redefines where value is generated in the pharmaceutical chain.
Behavioral Interoperability Is the True Future
Europe is building ambitious frameworks like the European Health Data Space (EHDS).
More information at: [[https://health.ec.europa.eu/ehealth-digital-health-and-care/european-health-data-space_en]
The strategic risk is clear: building a massive infrastructure of interoperable clinical data without integrating actual behavior. The future of European healthcare will depend not only on technical interoperability, but on behavioral interoperability. Because in the absence of this capability, shortages will not disappear: they will simply change form.
The question the sector does not yet dare to ask is not about supply. The real and urgent question is:
Who is going to interpret actual pharmaceutical demand in Europe… before the system reacts too late?
Whoever resolves this layer of operational interpretation —not production, not distribution, but behavioral intelligence— will not only reduce shortages. They will completely redefine the European health system.
Sources and Reference Frameworks
European Medicines Agency (EMA) – Availability of medicines in Europe. [[https://www.ema.europa.eu/en/human-regulatory/post-authorisation/availability-medicines]
European Commission – European Health Data Space (EHDS). [https://health.ec.europa.eu/ehealth-digital-health-and-care/european-health-data-space_en]
OECD – Health data and system performance. [https://www.oecd.org/health]
#EuropeanPharmacy #MedicineShortages #HealthTech #EHDS #BehavioralInteroperability #SupplyChain #DigitalHealth #HoyLunes #HealthStrategy #PharmaceuticalInnovation #EhabSoltan